Did you know that you could make a positive impact in people’s lives by working as a Business Analyst (BA)? By describing data flows, writing use cases, creating diagrams, re-engineering current processes or mapping the system’s data outputs and inputs, you could make a change in somebody’s life. As impossible as it sounds, it is happening on a daily basis. Throughout the US the Business Analysts in the Healthcare industry work hand in hand with the Healthcare professionals in the hospitals, the insurance companies, the government, as well as regulatory and non-profit agencies and organizations to make the US Healthcare better.
According to the MS Encarta Dictionary, healthcare is defined as the “activities to maintain health; the provision of medical and related services, aimed at maintaining good health, especially through the prevention and treatment of disease.” The healthcare industry also includes the people performing these activities, their skills, and the tools and systems they use daily. The modern health care depends on an ever growing interdisciplinary team of professionals; and this includes the Business Analysts.
The Business Analysts in the Healthcare Industry are exploring many business processes, multiple use cases and alternative flows at every point of contact where the patient interfaces with the healthcare professionals. At the same time there are various software and hardware systems interacting with each other and a multitude of standards regulating every aspect of the data exchange. When you add the different vendors, the variety may become overwhelming.
Where to Start?
There is no shortcut for learning all the intricacies overnight. The best approach for getting started is to focus on the current project or the company you work for. If your current area of interest is laboratory information systems for example, you may need to look into the different types of lab tests, their specific cut-off and interpretation variations, the laboratory workflow models, test equipment and lab information systems at the site, etc. On the other hand if the area of your project is health insurance, hospital administrative data, hospital information or billing systems, performance reporting or quality and safety improvement, you are more likely to become familiar with any part of the diagram below. It is a high level overview of the hospital stay process.
Click Image to View Larger Version
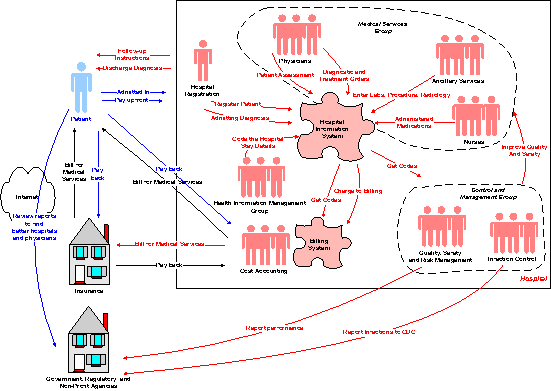
There are two elements that unite every item on the diagram: HL7, and HIPAA.
HL7 is a protocol developed to provide a standard for data exchange interfaces across various computer systems. It is developed by Health Level 7 (HL7), an accredited Standards development organization. HL 7 is part of ANSI. It operates in the healthcare arena and in particular in the clinical and administrative data domain. According to their website (www.hl7.org) the HL7’s mission is to provide “standards for interoperability that improve care delivery, optimize workflow, reduce ambiguity and enhance knowledge transfer among all of our stakeholders, including healthcare providers, government agencies, the vendor community, fellow Standards Developing Organizations and patients.”
HIPAA, the US Health Insurance Portability and Accountability Act, deals with the privacy and medical data transmission. At the website of the United States Department of Health and Human Services (http://aspe.hhs.gov/admnsimp/ ) you can find a general overview as well as the national standards for protecting the privacy of personal health information. Under HIPAA, Protected Health Information (PHI) is any information about the health status and the provision or payment of health care that can be linked to an individual. This broad interpretation includes any part of the medical record, or medical and payment history of the patient.
Hospital Systems: HIS and EHR
The compilation of the PHI starts when the patient is admitted to the hospital. The hospital registration personnel enter his demographic data and admission diagnosis into the Hospital Information System (HIS) or into the Electronic Health Record (EHR).
Both systems may store the following types of data:
- patient demographics;
- medical history like medicine and allergy lists or progress reports of illnesses;
- details for each episode of care like:
- laboratory test results;
- procedure and test appointments ;
- radiology images (X-ray, MRIs, etc.) and clinical photographs (endoscopy, laparoscopy, etc.);
- prescribed and administered medications.
Even more information is added throughout the hospital stay and even after the patient is discharged.
So what's the difference between HIS and EHR?
The difference is that the HIS, according to Wikipedia, is “a comprehensive, integrated information system designed to manage the administrative, financial and clinical aspects of a hospital” and also “encompasses paper-based information processing as well as data processing machines”, while the EHR “refers to an individual patient's medical record in digital format” and “may be made up of electronic medical records from many locations and/or sources.”
The Office of the National Coordinator for Health Information Technology (http://www.hhs.gov/healthit/chiinitiative.html) recommends the nationwide federal adoption of EHR standards in the US and the private, not-for-profit organization, Certification Commission for Healthcare Information Technology (www.cchit.org) evaluates and develops the certification for EHRs in the US.
Medical Services and Beyond
The medical services process for the patient starts with his admission to the hospital. During the hospital stay a team of physicians assesses him by ordering and then interpreting the results of his laboratory, radiology, and other data. After diagnosing the patient, the doctors order different treatments (medications, diets) and therapy. These orders are carried by the ancillary services personnel such as radiology and lab technicians, physical therapists, or hospital pharmacists; while the nurses administer the medications. As a result, the patient gets well (hopefully) and is discharged from the hospital with assigned discharge diagnosis and follow up instructions.
Here ends the medical services process flow from the patient point of view. However there is a lot more going on in the background. And there is where the Business Analysts is involved the most.
At the time these medical service activities are performed, their results and details are recorded in the HIS, in the patient chart, or in the EHR, depending on the specific setup at the medical facility.
The Control and Management group in the hospital controls the provision of medical services by:
- ensuring the physician, department, and hospital performance improvement;
- managing the risk and monitoring for hospital acquired infections;
- running control, trend, comparison and other types of reports by physician, specialty;
- etc.
This group could have multiple departments like: Quality Control, Case Management, Performance Improvement, Infection Control, Risk Management, or Safety Management.
After the patient is discharged from the hospital the medical coders from the Health Information Management group, another group not visible to the patient, start coding the administrative data collected by the hospital during the patient stay. Health information coding is the encoding of verbal and verbose descriptions of diseases, injuries, and procedures into numeric or alphanumeric designations. This data describes the general characteristics of the hospital stay: patient’s age, length of stay, diagnoses, procedures, medications, etc.
The medical coders utilize standard codes, groups and categories that ensure the uniformity of the data coming out of the hospitals. This way, organizations responsible for the reimbursement of the medical services could set standard payments for certain procedure codes. These standard codes enable the generation of uniformed medical services, medical specialty or hospital reports, and the creation of statistics at state and federal level.
The medical coders utilize the standard uniform bill (UB04). The UB04 specification is maintained by the National Uniform Billing Committee (NUBC). According to their website (www.nubc.org), they were formed “to develop a single billing form and standard data set that could be used nationwide by institutional providers and payers for handling health care claims”. Recorded webinars, web-based courses and plenty or articles on this topic could be found on the UB04 KnowledgeTrek website (http://www.ub04.net/).
In addition, the health information management specialists utilize ICD codes to record the procedures performed and the diagnosis assigned. The International Classification of Diseases (ICD) provides up to six character long codes for disease, signs, symptoms, external causes of injury, etc. classification. The most widely used version in the US in ICD-9-CM. Its yearly updates are published in the Federal Register on October 1st and affect both the diagnosis and the procedure codes. The updates since 1998 are available on the IRP, Inc. website (http://www.drg.irp.com/feds.htm).
Based on the ICD diagnosis and procedure codes from the patient record, and the patient’s demographic data, the diagnoses are additionally organized in over 500 Diagnosis-Related Groups (DRG) by a “grouper” program. Medicare (www.medicare.gov) updates the DRGs every October. The current version is V25 from October 2007. These DRGs are further grouped into Major Diagnostic Categories (MDC) that correspond to a single organ system and in general are associated with a particular medical specialty.
Reporting
Once organized by the medical coders, the health information is submitted by the hospital Cost and Accounting department to Medicare, Medicaid, private insurance companies, etc. for reimbursement for the medical care. The hospital Quality Department on the other hand, submits data to government, regulatory and non-profit organizations for public reporting and analysis. Among those organizations are the Joint Commission, the American Medical Association and state health agencies.
The government, regulatory and non-profit agencies and organizations, that collect hospital data, in addition to statistical data, offer hospital performance reports to help people identify the best hospitals for their case. All of them have plenty of information on their web-sites. For example the Center for Medicare and Medicaid Services web-site (www.cms.hhs.gov) offers guidelines and information organized by topic or provider type, and a Medicare Learning Network for Medicare and Medicaid related information.
The Joint Commission had recently sponsored a collaborative forum WikiHealthCare which in their words will “foster collaboration among tens of thousands and in due course of time millions of health care professionals”.
More Resources
Health management information can be found on the American Health Information Management Association website (www.ahima.org). This organization offers webinars, online documentation, and training staying true to its mission “To be the professional community that improves healthcare by advancing best practices and standards for health information management and the trusted source for education, research, and professional credentialing.” They also have a glossary of health information management terms found at: http://himcareers.ahima.org/whatishim3a.html.
Alternatively you could check the web-sites of your medical insurance providers and state health agencies, or you could subscribe to “Advance”, the magazine for health information professionals.
Tests and Certifications
If you are looking for an official recognition of your knowledge in the Healthcare area, you could get certified at www.brainbench.com. The tests are performed online and consist of multiple choice questions. At the end you will receive a printed certificate and a transcript number that will allow online verification of your credentials. This website offers certification tests in Healthcare Administration (US), Healthcare Industry Knowledge (US), Health Insurance, HIPAA (both privacy and security), Medical Billing, Medical Terminology, etc. It also offers pre-hire tests for employers, and has several case studies available on this topic.
On the other hand, if you are planning on getting a healthcare information related degree, obtaining an RHIA (Registered Health Information Administrator) certification from AHIMA might be an added bonus. According to AHIMA, the “professionals holding the RHIA credential are skilled in the collection, interpretation, and analysis of patient data. Additionally, they receive the training necessary to assume managerial positions related to these functions.” Among the requirements is to “ successfully complete the academic requirements, at the baccalaureate level, of a health information management (HIM) program accredited by the Commission on Accreditation of Health Informatics and Information Management Education (CAHIIM) “. The CAHIIM website has a directory of accredited HIM education programs at the masters, baccalaureate and associate degree levels in all states.
* NOTE: This article does not claim to provide an exhaustive list of participants, standards, organizations, online resources, etc. All URLs correct at time or publishing.
Author: Vessela Neytcheva, PMP is a business analyst in the clinical information management group of Cardinal Health (www.cardinal.com).